The rise of antibiotic resistance has pushed scientists to revisit a century-old idea: using viruses to kill bacteria. Phage therapy once overshadowed by antibiotics is now gaining global traction as a personalized, precision weapon against stubborn infections. While challenges remain, groundbreaking advances in research, regulatory shifts, and compelling patient success stories are breathing new life into this innovative treatment.
What is Phage Therapy?
Bacteriophages (or phages) are viruses that naturally infect and destroy specific bacteria. Discovered over a century ago, they exist abundantly in nature in soil, water, and even the human gut. Phage therapy harnesses these microbes to target bacterial infections with remarkable precision, offering a tailored alternative to broad-spectrum antibiotics.
Why Phage Therapy Matters Now
Antibiotic resistance is projected to cause 10 million deaths annually by 2050 if left unchecked. Phage therapy addresses this crisis through:
- Surgical Precision:
Phages attack only their target bacteria, sparing beneficial microbes. This specificity minimizes collateral damage to the microbiome, reducing side effects like diarrhoea or yeast infections common with antibiotics. - Combating Resistance:
Unlike antibiotics, phages evolve alongside bacteria, adapting to overcome resistance. While phage resistance can occur, researchers mitigate this using “cocktails” of multiple phages or pairing phages with antibiotics for synergistic effects. - Personalized Medicine:
Each phage is matched to a patient’s unique bacterial strain, enabling bespoke treatments. Advances in DNA sequencing and AI now accelerate phage selection, making personalized therapy faster and more accessible. - A Century of Safety:
Used safely since the 1920s in Eastern Europe, phages have minimal side effects. Modern purification techniques and clinical trials continue to validate their safety profile.
Global Progress: From Compassionate Use to Approved Drugs
While phage therapy remains experimental in most countries, recent milestones signal a turning point:
- Belgium: In 2023, the country approved the first standardized phage therapy, Pyophage, for UTIs and wound infections.
- USA: The FDA’s Expanded Access Program allows compassionate use for life-threatening infections. Companies like Adaptive Phage Therapeutics are advancing clinical trials for diabetic foot infections and prosthetic joint infections.
- Australia: Phage Australia has treated over 20 patients under compassionate access, with a 2023 study showing 85% success in chronic infections.
- Georgia & Poland: Clinics like the Eliava Institute in Tbilisi and the Ludwik Hirszfeld Institute in Wrocław continue pioneering treatments for antibiotic-resistant infections.
However, regulatory hurdles persist. In the U.S., phages are not yet FDA-approved drugs, though the 2023 TAGS Act aims to fast-track antimicrobial solutions like phage therapy.
Success Stories: When Antibiotics Fail
Recent cases highlight phage therapy’s lifesaving potential:
- Lung Transplant Breakthrough (2023):
A patient with a multidrug-resistant Pseudomonas aeruginosa infection received a customized phage cocktail via nebulizer and IV. Within weeks, the infection cleared, marking a milestone in treating lung infections. - Chronic Prosthetic Joint Infection:
A 68-year-old with a 2-year Staphylococcus epidermidis infection saw complete resolution after phage therapy combined with antibiotics, avoiding limb amputation. - Tom Patterson’s Legacy:
The UC San Diego professor, whose 2016 MRSA cure popularized modern phage therapy, continues advocating for research. His case inspired the creation of the IPATH (Innovative Phage Applications and Therapeutics) Centre. - Pediatric Triumphs:
In 2024, a 6-month-old with cystic fibrosis and a Burkholderia infection recovered after phage therapy, underscoring its potential for vulnerable populations.
Challenges and Innovations
Phage therapy isn’t without obstacles:
- Regulatory Complexity: Each personalized cocktail requires separate approval.
- Manufacturing: Scaling production while maintaining quality is costly.
- Phage Resistance: Bacteria can develop resistance, necessitating dynamic treatment adjustments.
Researchers are tackling these issues with:
- Engineered Phages: Companies like Eligo Bioscience are CRISPR-editing phages to enhance efficacy.
- Phage Databases: Platforms like Phage Directory and GPHAP (Global Phage Hub) crowdsource phages for rapid matching.
- Synthetic Biology: Hybrid “phage-antibiotic” conjugates (e.g., SPARKI™) combine phages’ targeting with antibiotics’ killing power.
The Future of Phage Therapy
2024 is poised to be a watershed year. Key developments include:
- Phase III Trials: Results from APT’s PHAGE Trial for Staphylococcus aureus infections.
- AI-Driven Discovery: Startups like Felix Biotechnology use machine learning to predict phage-bacteria interactions.
- At-Home Testing: DIY phage kits (still in beta) could someday let patients screen phages against their infections.
Phage therapy is no longer a relic of the pre-antibiotic era—it’s a cutting-edge solution for the post-antibiotic world. With its precision, adaptability, and growing clinical validation, phages offer hope where antibiotics fall short. While challenges like standardization and access remain, collaborations between scientists, regulators, and patients are paving the way for a future where phage therapy is mainstream.
As research accelerates, one thing is clear: the tiny viruses that once dwelled in sewage and soil may soon revolutionize how we treat infections—one bacterium at a time.




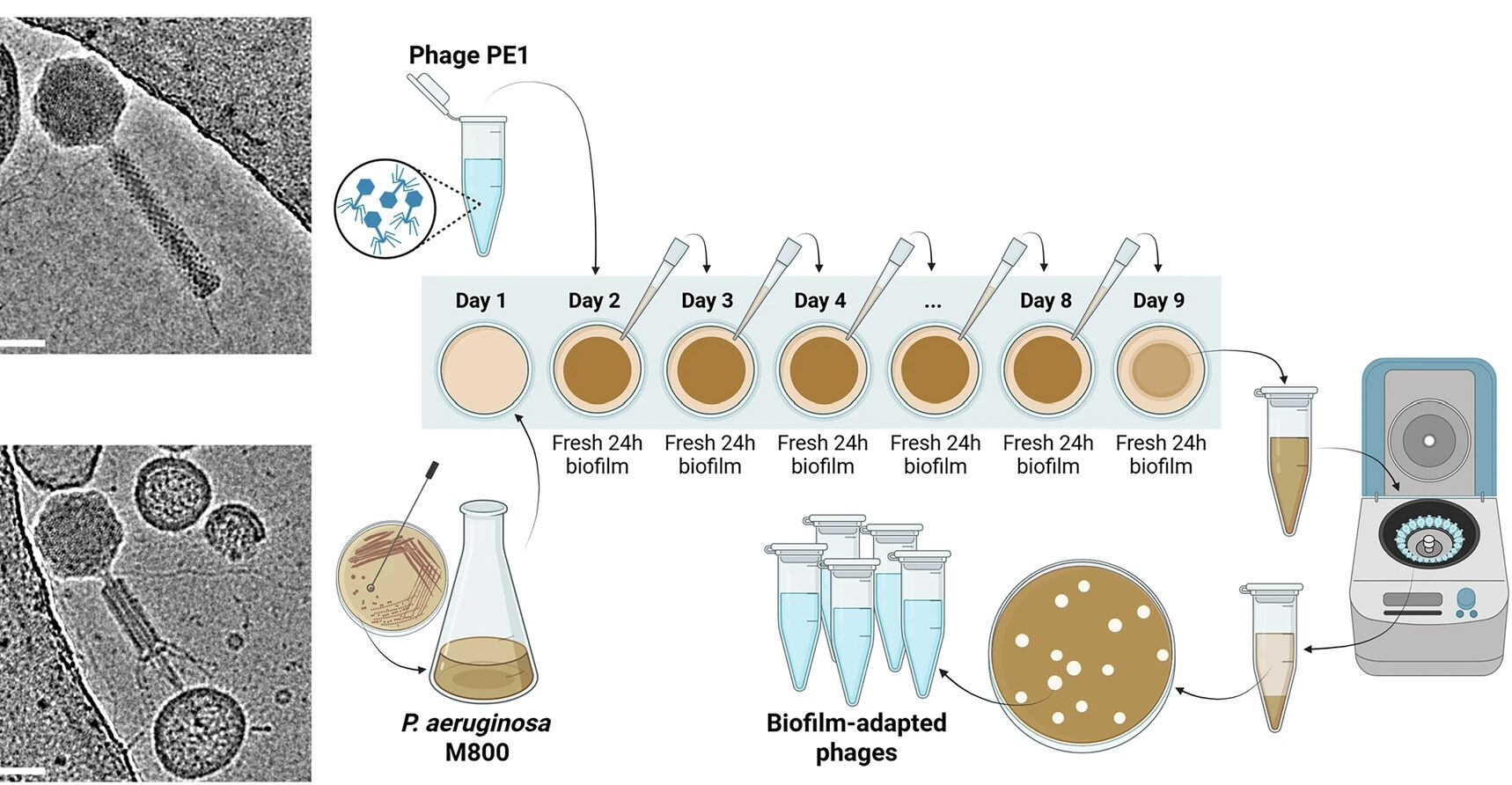
[…] research has seen a resurgence in recent years due to its potential for treating antibiotic-resistant bacteria. One of the critical ways to study phages is through visualization under a microscope. Microscopy […]
[…] cocktails are an innovative solution for treating bacterial infections. They are a mixture of two or more purified bacteriophages, which are viruses that infect bacteria. […]
[…] human’s natural curiosity, the discovery of bacteriophages capable of clearing bacterial infections has prompted widespread interest in the possibility of […]
[…] research has seen a resurgence in recent years due to its potential for treating antibiotic-resistant bacteria. One of the critical ways to study phages is through visualization under a microscope. Microscopy […]
[…] case highlights a groundbreaking development: the successful use of bacteriophage therapy to control chronic infections in a patient with Netherton Syndrome. Bacteriophages, or phages, are […]
[…] have developed a novel method to significantly boost the effectiveness of bacteriophage therapy, a promising alternative to antibiotics for treating bacterial infections. By encapsulating […]
[…] Phage Therapy: A Personalized Approach to Treating Bacterial Infections […]
[…] develop an AI model. With this AI model, performing phage-host matching becomes a lot easier. The phage therapy currently involves isolating specific phages from the environment, identifying those effective […]
[…] change reflects its transition from a research-oriented organisation to one focused on delivering phage-based therapies for clinical use. According to the company, the goal is to support healthcare professionals with more precise, […]
[…] change reflects its transition from a research-oriented organisation to one focused on delivering phage-based therapies for clinical use. According to the company, the goal is to support healthcare professionals with more precise, […]
[…] recently published an article that examined how phage therapy worked in a randomised clinical trial. A Belgian consortium conducted an observational study of […]